Myomas and their implications on female infertility
A uterine myoma is the most frequent benign tumour in the female reproductive system. It would be very rare for a uterine myoma to become malignant. A myoma is a tumour made of smooth muscle cells and is also known as a fibroma, leiomyoma or fibromyoma.
Females are approximately 40%-50% likely to develop a myoma over the course of their reproductive years.
What can cause myomas?
Risk factors for developing myomas include biological inheritance, race (myomas are more frequent in Black women), obesity, being close in age to menopause and high levels of oestrogen and progesterone.
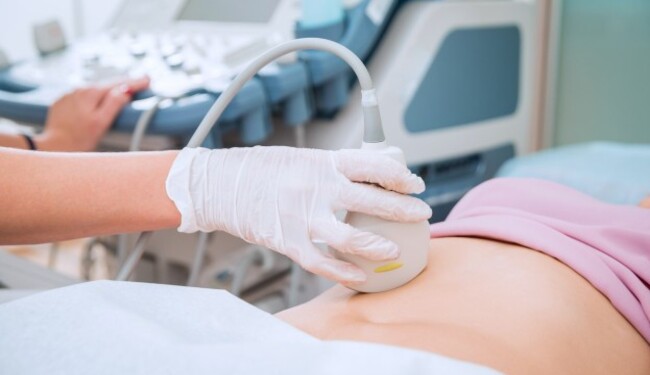
Diagnosing a myoma is done by performing a physical examination, an endovaginal ultrasound and an abdominal ulrasound, which are considered to be the “gold standard” of myoma diagnosis and monitoring. The transvaginal ultrasound is about 95-100% accurate when it comes to detecting small uterine myomas.
A diagnostic hysteroscopy may also be necessary: this is the technique of choice for assessing submucosal and intracavitary myomas so that a surgical approach can be evaluated. Finally, an MRI is the best imaging tool to determine the size and location of a myoma, although it’s also the most expensive. It’s generally the test of choice to assess a surgical indication or to diagnose adenomyosis and/or sarcomas.
What relationship is there between myomas and infertility?
Myomas can be found in 5-10% of patients battling infertility, but sterility or infertility caused by myomas is a controversial topic which is still under discussion. It is only recognised as the sole cause of infertility in less than 3% of cases.
At present there is a consensus that the location of myomas within the uterine cavity is a key factor when it comes to their negative impact on fertility. Myomas that distort the uterine cavity (submucosal or intramural myomas with an intracavitary component), make it more difficult to conceive and also increase the likelihood of miscarriage.
The mechanisms which cause infertility would be:
Interference in gamete transport:
- Abnormal cervical anatomy
- Stretched and deformed uterine cavity
- Obstruction of the entrance to the fallopian tubes
- Fallopian tube or ovarian deformities that interfere with catching the released egg
- Increase in uterine contractions
Implantation failure:
- Distortion of endometrial blood vessels
- Secretion of intracavitary fluids
- Secretion of vasoactive substances and local inflammatory factors
- Increased estrogen levels in the endometrium
- Increase in uterine contractions
There are several classifications for myoma location. The location of a myoma is the factor that has the greatest impact on fertility. Intracavitary and/or submucosal myomas are associated with reduced fertility and an increased risk of miscarriage (NE: Ib-A). Intramural myomas may be associated with reduced fertility and greater chances of miscarriage (NE: III). Finally, subserosal myomas do not seem to have any impact on reproductive outcomes (NE: III).
In terms of the rest of the parameters to be assessed, such as myoma size and/or number, their etiological role in infertility is still unclear and the management of intramural myomas is the topic that sparks the most debate.
Treatment for uterine myomas and fertility
When treating a myoma has been advised, the treatment of choice is surgical intervention (generally performed through laparoscopy, abdominal surgery or hysteroscopy depending on its location), rather than medical or expectant management.
With the evidence that is currently available, there is debate around the advantages of treating intramural myomas in patients with unexplained infertility or recurrent miscarraige. However, there is more evidence in favour of treating them.
This is because the myomectomy by hysteroscopy significantly reduces the risk of miscarriage in these women compared to those who opt for expectant management. In addition, pregnancy rates are higher after a myomectomy in women who are not dealing with any other infertility issues.
At present, new treatments are being utilised for women with a history of miscarriage and intramural myomas to improve pregnancy rates, such as HIFU/MRgFUS, laparoscopic or transvaginal radiofrequency volumetric thermal ablation (RFTVA), but clinical evidence has not yet been seen.
Have you been diagnosed with a uterine myoma and are you concerned about your fertility? Request an appointment with us to discuss your case and we’ll do everything possible to help you.

