What is the testicular biopsy in assisted reproduction?
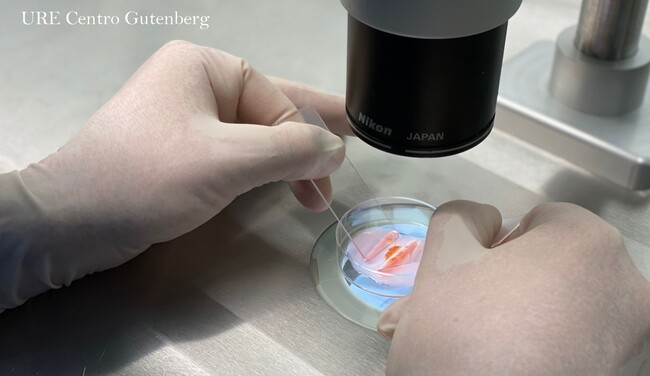
The testicular biopsy is one of the surgical procedures that we perform at URE Centro Gutenberg on males whose semen samples from ejaculate do not contain spermatozoids.
With this in mind, and as you may imagine, the purpose of this procedure is to obtain spermatozoids to be used for in vitro fertilisation with ICSI regardless of whether the fresh sample will be used, or rather frozen to be used at some point in the future.
What does the testicular biopsy involve?
The testicular biopsy is a simple surgical intervention that is performed in the operating theatre using local or general anaesthesia. The procedure takes approximately 20 to 30 minutes.
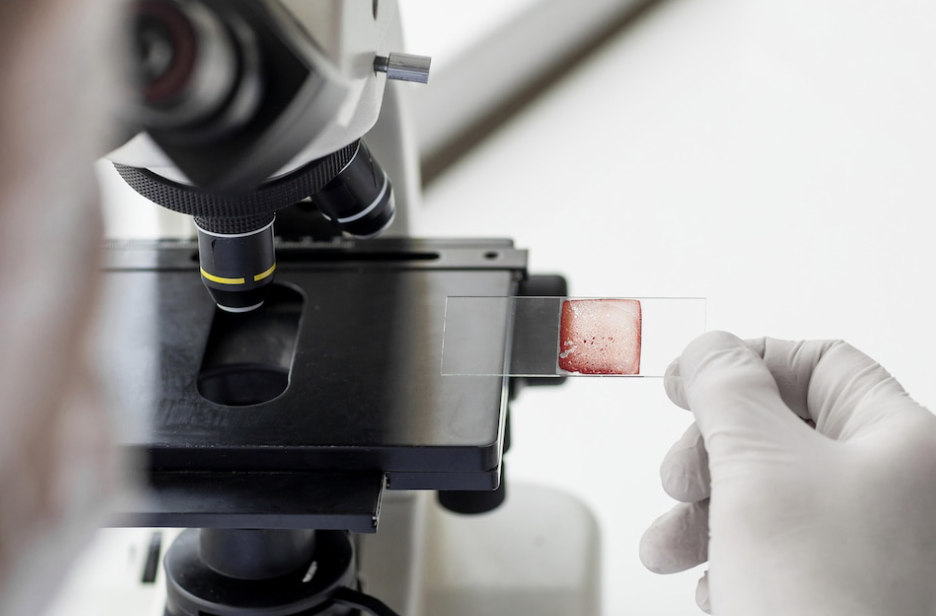
The technique is carried out by making a small incision through the skin of the scrotum. Once the surgeon has reached the testicle, generally the right one, a small sample of testicular tissue is extracted. This sample is immediately evaluated under a microscope in order to confirm the presence of spermatozoids, as well as their motility.
As we were saying before, the spermatozoids that are retrieved can be used while fresh in a cycle of IVF/ICSI the same day the eggs are collected. This is known as a synchronous testicular biopsy. It is also possible to freeze the sample and use it in the future, known as asynchronous testicular biopsy.
In the event that no spermatozoids are found, the biopsy is performed on the other testicle during the same surgery. Additionally, part of the sample can be used to run an anatomic pathology study to help provide the patient with a diagnosis.
The testicular biopsy is an outpatient procedure, meaning the patient will be able to go home the same day and will be advised to remain relatively relaxed for the next 2 to 3 days. The incision site sutures will fall off on their own or can be removed after about 15 days.
When is a testicular biopsy recommended?
In assisted reproduction this procedure is indicated when we need to study patients with an azoospermia diagnosis. In other words, when no spermatozoids are found in the semen from ejaculate, this procedure is requested to help confirm secretory azoospermia or obstructive azoospermia. It is also possible to utilise this procedure in some cases where there is an extremely low number of spermatozoids in the ejaculate, a condition referred to as cryptozoospermia.
Aside from these cases, testicular biopsies are also performed on males who have previously undergone a vasectomy (surgical tying of the vas deferens), and who now wish to have more children, as well as on males who have trouble ejaculating due to physical or psychological issues.
What risks are associated with the testicular biopsy?
As with any medical intervention this procedure is not risk free, though the associated risks tend to occur very infrequently. The most common risks are local haematoma, infection and/or inflammation of the testicle, epididymis or scrotum, allergic reaction to the medication or sutures used, etc.
Patients must always be aware that it is possible that no spermatozoids will be found in the testicular tissue that has been biopsied. In these cases, the alternative is to use sperm from a donor sperm bank. At URE Centro Gutenberg this potential outcome is always discussed with the patients before performing the testicular biopsy so that the couple is fully informed ahead of time.
We hope we have helped you to know what this small intervention at URE Centro Gutenberg is. As always, we’re here to answer any questions you may have and to assist you with anything else you may need.
You can request an appointment with our assisted reproduction specialists or send your question by clicking here.